James Faber works on blood vessels that are as useful as the appendix is for everyday life. But when the cardiovascular system malfunctions, these vessels — called collaterals — form a backup system that can mean the difference between life and death.
Collaterals are just plain weird. They’re rare: there may be only one collateral vessel for every thousand arteries, capillaries, and veins in the human circulatory system. And they’re tiny — nearly a hundred times smaller than an average artery. Instead of following the standard artery-to-capillary-to-vein route, they connect groups of arteries called artery trees. There’s also little, if any, net blood flow through collaterals under normal circumstances. And an even more bizarre feature is that in collaterals blood can flow in both directions. According to Faber, people could survive perfectly well under normal circumstances without any collaterals at all. Yet people with more collaterals have a better chance of surviving a heart attack or stroke. And Faber wanted to know why.
During World War II, cardiac surgeon Michael Debakey noticed that some soldiers who had received wounds that obstructed major arteries in their arms or legs had to have amputations, but others didn’t despite having similar injuries. Debakey thought that blood was bypassing the blocked arteries by traveling through collaterals, and that the soldiers who could still use their arms and legs simply had more collaterals. Faber and other scientists thought that something similar could be happening when a clot or a cholesterol plaque cuts off blood flow.
Still, the idea that some healthy people have more collaterals than others has been difficult to prove. The only direct method for determining the number is to count them — postmortem. Even then, finding collaterals isn’t easy. And to estimate the number of collaterals in a living person, researchers have to insert a device into a person’s heart, a risky procedure. “Right now, we can’t tell whether the difference in the number of collaterals comes from genetics or the environment,” Faber says. “You don’t know how many of those people were exercisers or ate too many cheese nachos.”
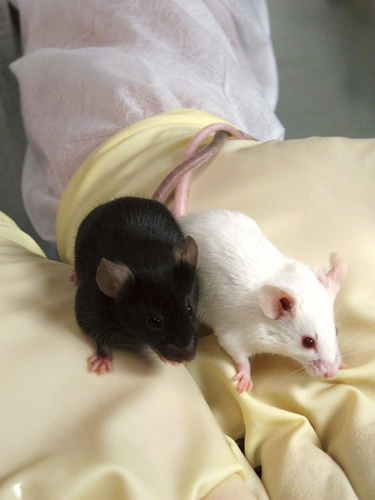
So Faber decided to use mice. Other scientists had identified two strains of mice that recovered very differently after an artery was blocked in their legs. Blood flow in the BALB/c strain, an albino strain, recovered more slowly and had more tissue damage compared to another strain called C57BL/6, also known as the black-six strain. The scientists noticed that the collaterals expanded more in the black-six strain than in the albino strain after an artery was blocked, and concluded that that was why the black-six strain healed faster. That conclusion bothered Faber. When he examined the data, he was convinced that the difference in expansion couldn’t explain the faster recovery of the black-six mice unless they had more collaterals to begin with.
Faber wanted to repeat the study and improve it. But he needed to find a better method for counting collaterals. The earlier study had examined the thigh muscle, but there are only ten to twenty collaterals in a mouse’s thigh. The methods to find these rare vessels in muscle were not easy or very reliable. There had to be a better way.
“We were driving back from a meeting in Washington, D.C.,” Faber says. “I was sitting in the back seat of the car and I was thinking: What tissue has its circulation laid out in two dimensions where you can really see everything? I thought of the retina, but it doesn’t have collaterals. Then it hit me — the cerebral cortex.”
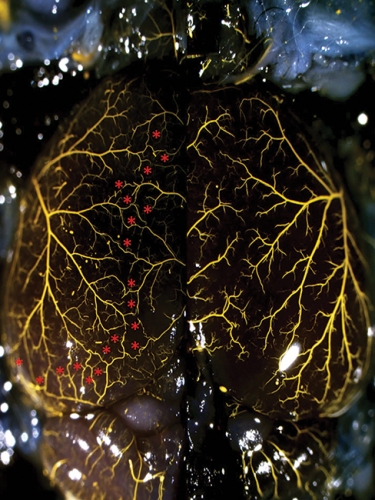
The cerebral cortex requires a constant supply of blood. But the major blood vessels for the brain don’t enter the brain itself: instead, they sit on its surface and send tiny branches inside so that valuable brain space isn’t taken up by larger blood vessels. Faber realized by using the mouse cortex as a model, they could take pictures of the vessels without having to dig through brain tissue.
When Faber and his students returned from their meeting, they injected the albino and black-six mice with fluorescent barium sulfate. They used barium sulfate crystals that were small enough to pass through larger blood vessels, including collaterals, but that were too big to pass through the smaller blood vessels that traveled into the brain and into the capillaries and veins. The result was a set of clear images that showed that the black-six mice had lots of collaterals while the albino mice had very few. Faber’s group also found similar differences in the thighs and intestines. But why did the black-six mice have more collaterals than the albino mice?
“They live in the same environment,” Faber says, “eat the same food, drink the same water and have the same bedding. The environment was controlled, so we concluded that the difference must come from their genetic background.”
The hunt was on for the genes that controlled collateral formation. To narrow down their search, Faber selected fifteen mouse strains, including the albino and the black-six strains, to represent genetic diversity. His lab members counted the collaterals in the cerebral cortex. The number of collaterals varied widely among the fifteen strains. But they also found a new pattern: the mice that were genetically similar to the albino mice had fewer collaterals, and the mice that were genetically similar to the black-six mice had more. There was a physical trend, too: Faber and his team noticed that the mice with a small number of collaterals had more severe strokes than the mice that had a high number of collaterals.
To figure out which genes are associated with the number of collaterals, Faber’s group bred the albino mice with the black-six mice. Then they interbred the hybrid mice once more to create a new generation with more genetic variety. They counted collaterals in each mouse and then searched for genes linked to the number of collaterals. Out of the thousands of genes they investigated, Faber’s group found four that were connected to the number of collaterals. They decided to focus on the one that showed the strongest connection in both mouse strains. This allowed them to narrow down their search from more than thirty thousand genes to only nine.
The nine genes that Faber’s team uncovered have no known connection to blood vessel formation. The next step will be to test whether these genes are involved in building collaterals. But Faber is also hoping that their findings will eventually translate to humans. Knowing the genetics behind collateral formation could lead to better treatments for vascular diseases.
“We could genetically screen people inexpensively and see how many collaterals people have to determine their risk for vascular diseases,” Faber says. Having a screen could also improve tests for new drugs that target collaterals. Some scientists are attempting to make drugs that cause collaterals to expand and let more blood flow. But, Faber says, if these types of drugs were tested on people who have few collaterals in the first place, then researchers wouldn’t be able to tell whether the drugs were effective.
According to Faber, another way to tackle the problem would be to create drugs that form more collaterals and redirect blood around blocked vessels. Faber’s lab has found that collaterals form late in gestation, well after the general circulatory system has already been established in the fetal mouse. And once the collaterals are there, no new ones form. Faber’s still working out the details, but he says that his team has identified two genes that trigger collateral formation, and they are searching for more.
There is also the question of how collaterals escape the process that normally prunes away unnecessary or malfunctioning blood vessels that have little or no net flow. Faber thinks that the cells that line the inside of the collaterals — called endothelial cells — are different from those in other blood vessels, which could mean that collateral endothelial cells somehow defy the signals that mark redundant blood vessels for elimination.
There’s still a lot to learn about these tiny, bizarre vessels. Faber says he and his lab aim to pursue this vascular puzzle until it’s finished. He is continually fascinated by collaterals and amazed that vessels that are normally useless in healthy individuals can actually save lives. “That’s a big deal for accessory vessels that you ordinarily don’t need,” he says.
Meagen Voss received a master’s degree in neurobiology in spring 2010.
James Faber is a professor in the Department of Cell and Molecular Physiology in the School of Medicine. This work has been published in Physiological Genomics, Circulation Research, and Journal of Cerebral Blood Flow and Metabolism. Funding came from the National Institutes of Health.