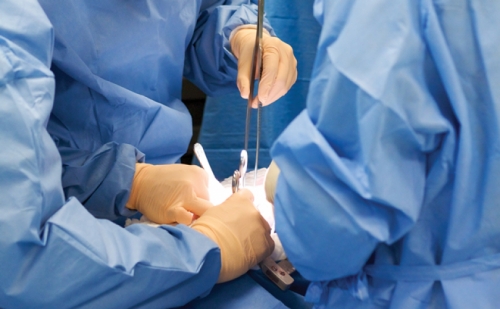
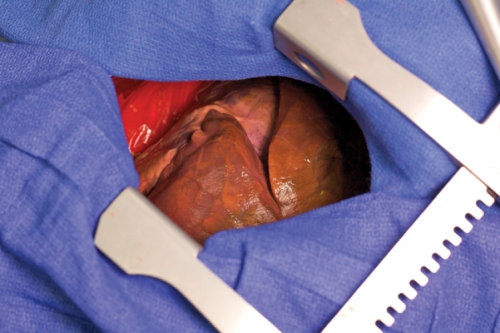
An operating room: bright lights, trays of instruments, people in masks and blue gowns. A monitor on the wall shows a live image of a patient’s heart. The resident standing next to the operating table has just performed an artery bypass graft; he’s waiting while the more experienced surgeon who guided him through the procedure inspects his work.
Good job, the surgeon tells him. Now do it again—this time, with the heart beating.
The heart is from a pig, and the patient is an old mannequin from a clothing display. The blood inside it is fake, from a store that supplies it to Hollywood studios. But this is real training for residents specializing in cardiothoracic surgery. The heart is positioned in the mannequin’s chest like it would be in a human’s. It can produce arrhythmias if a surgeon in training handles it the wrong way, or when a computer tells it to. It can go into cardiac arrest. It’s not forgiving of mistakes. “If you don’t do the right thing,” surgeon Rick Feins says, “there’s going to be blood all over the place.”
Feins heads up a team that trains residents in common procedures such as coronary bypass, heart valve replacement, and lung resection. Simulators like this one aren’t part of the traditional curriculum for surgeons specializing in cardiothoracics; the surgical community hadn’t seen anything like it until Feins started using it in 2008. “At that time, no one in cardiac surgery really thought there could be anything that was like learning in the operating room,” he says.
Feins first started thinking about simulation in 2007, when one of his sons was in medical school and the other was training to be a navy pilot. Before Jonathan could get into a plane, he had to log hundreds of hours in a simulator. Wouldn’t it make sense, Feins thought, for surgical residents to have to do the same before they were allowed in the OR?
He started researching cardiac simulation, and at first the results didn’t seem too promising. Plastic models of the thorax (the organs in the chest) cost a lot and aren’t all that much like the real thing. Digital simulation is also expensive, and it lacks haptics—the quality of weightiness that tissue has when you pull on it. Sometimes surgical residents learn on live pigs, but that means killing a pig in order to practice with organs that aren’t even arranged like human anatomy.
But then Feins found a journal article about a cardiac simulator, complete with a video of it in action. It really looked like surgery being done on a human. He tracked down the article’s first author and called him up. “This is Dr. Feins. I’m from UNC and I’m the chair of the American Board of Thoracic Surgery. I read about your simulator, and I’d like to come down and see it.”
Is this a joke? Paul Ramphal asked. The article was two or three years old, and Feins was the first person to contact him about it. Ramphal, also a surgeon, had since moved on to other things. He’d also moved from Jamaica, where he built the simulator, to the Bahamas; all he had left of it were a few pieces sitting in his garage.
So come to Chapel Hill, Feins said. Bring anyone you need with you, and we’ll rebuild it here. They had only a small grant, but they made it stretch, getting free pig hearts from a North Carolina farm and scavenging old surgical equipment discarded by UNC Hospitals. Residents volunteered their time and labor (it turned out that they weren’t allowed to work for free under the terms of their contract, so they got minimum wage). When it was done, Feins took the simulator to a conference of cardiothoracic residents, where it was a hit.
“All it takes is for other surgeons to see the thing, and they say, ‘Wow, this is it,’” Feins says. “Most of them haven’t even really seen it—they’ve just seen our videos, and I get one or two calls a week asking where they can get one.” The University of the West Indies in Mona, where Ramphal first designed the simulator, is producing it for commercial sale; seven major hospitals, including Johns Hopkins and the Mayo Clinic, have already bought in. Meanwhile, Feins has led a yearly surgical boot camp at UNC, bringing residents from around the country along with surgeons to teach them.
Then in 2009, Feins and his colleagues designed a new simulator focused on the lungs. It’s also made of pig parts—heart, lungs, esophagus, and so on—arranged like they would be in a human. The lung simulator started when a biomedical engineering student from Vanderbilt, Alec Grubbs, came to work for Feins for the summer. Grubbs’s father, Andy Grubbs, was also an engineer, and happened to be a lecturer in the Kenan-Flagler Business School. The father-and-son Grubbses came up with solutions to make a lung simulator run cheaply—it has to look as realistic as the Ramphal simulator, but in this case, the heart simply has to beat while a student operates on the lungs.
They used a motor designed to power the windshield wipers of a car to drive a puff of air into the heart seventy-eight times a minute—the same rate at which a human heart might beat.
Andy Grubbs is starting a spin-off company to develop the lung simulator commercially. He and Feins want to produce it in rural North Carolina, where unused pig organs are plentiful and jobs are needed. They’re patenting a dummy that has removable sections that surgeons can replace with the organ systems they need, such as the liver, spleen, and kidneys (also made from pig parts). The U.S. military is interested in the dummy as a training tool for medics and Hospital Corpsmen.
Feins is also working on a curriculum to make surgery simulators part of the standard program for surgical residents. The traditional education that takes place in the operating room is safe for patients, he says, but it’s not the best way for residents to learn. “Operating rooms nowadays are very, very busy,” he says. “Teaching may not be as easy to do there as it was before. And in the operating room you can’t control the curriculum—whatever the patient has that day is what you’re teaching. That’s particularly difficult with what we call adverse events, because you can’t know when those will happen or inflict them at any time.”
Also, Feins says, in the OR you can’t practice a skill over and over the way you’d practice swinging a golf club or playing a piece on the flute. Surgical simulation could relieve some of the pressure on operating rooms by delivering residents who already have basic skills from working with real tissue.
“If you can teach those things in a controlled environment before you move on to the operating room,” he asks, “then why would you want to do it any other way?”
Richard Feins is a professor of surgery in the School of Medicine. The Ramphal Cardiac Surgery Simulator was built with funding from UNC’s Department of Surgery and the American Board of Thoracic Surgery. UNC medical students Matthew Dedmon, Melissa Readio, and Aaron Webel; UNC surgical residents Leora Tesche and Phil Pepple; and Vanderbilt engineering undergrad Alec Grubbs helped develop the Thoracic Surgery Simulator.
Watch more videos from UNC Health Care here.